Memory Care Experience
An experience that improves care outcomes for Alzheimer’s patients, caregivers and providers
Client
Advocate Aurora
Role
Lead Service & Interaction Designer
Industry
Healthcare
Focus
Vision Strategy & Concept
The Challenge
Advocate Aurora Health is a not-for-profit health care system looking to develop an actionable, research driven future memory care experience that focuses on driving improved outcomes, higher quality care, lower costs and an improved experience for members, their caregivers and the Advocate Aurora care team. The project focused specifically on Alzheimer’s disease patients in Wisconsin and Illinois.
Research
To understand the complex Alzheimer’s ecosystem, I conducted deep empathy interviews with seven patients, six caregivers, and five providers with the goal to map the lived experiences and unmet needs within existing care models and identify the specific friction points that define the journey from diagnosis onward. This research culminated in the development of four distinct user archetypes, based on priority on independence vs relationships and identity in doing vs remembering.
Diagnosis
Alzheimer’s diagnosis is doubly delayed - first by patients, then providers.
Care Plan
The most impactful care happens when families look beyond the doctor’s office.
Care Plan
Continuity in care falls on caregivers and secondary providers.
Care Plan
Living with Alzheimer’s is a team sport, but the plays don’t include all the players.
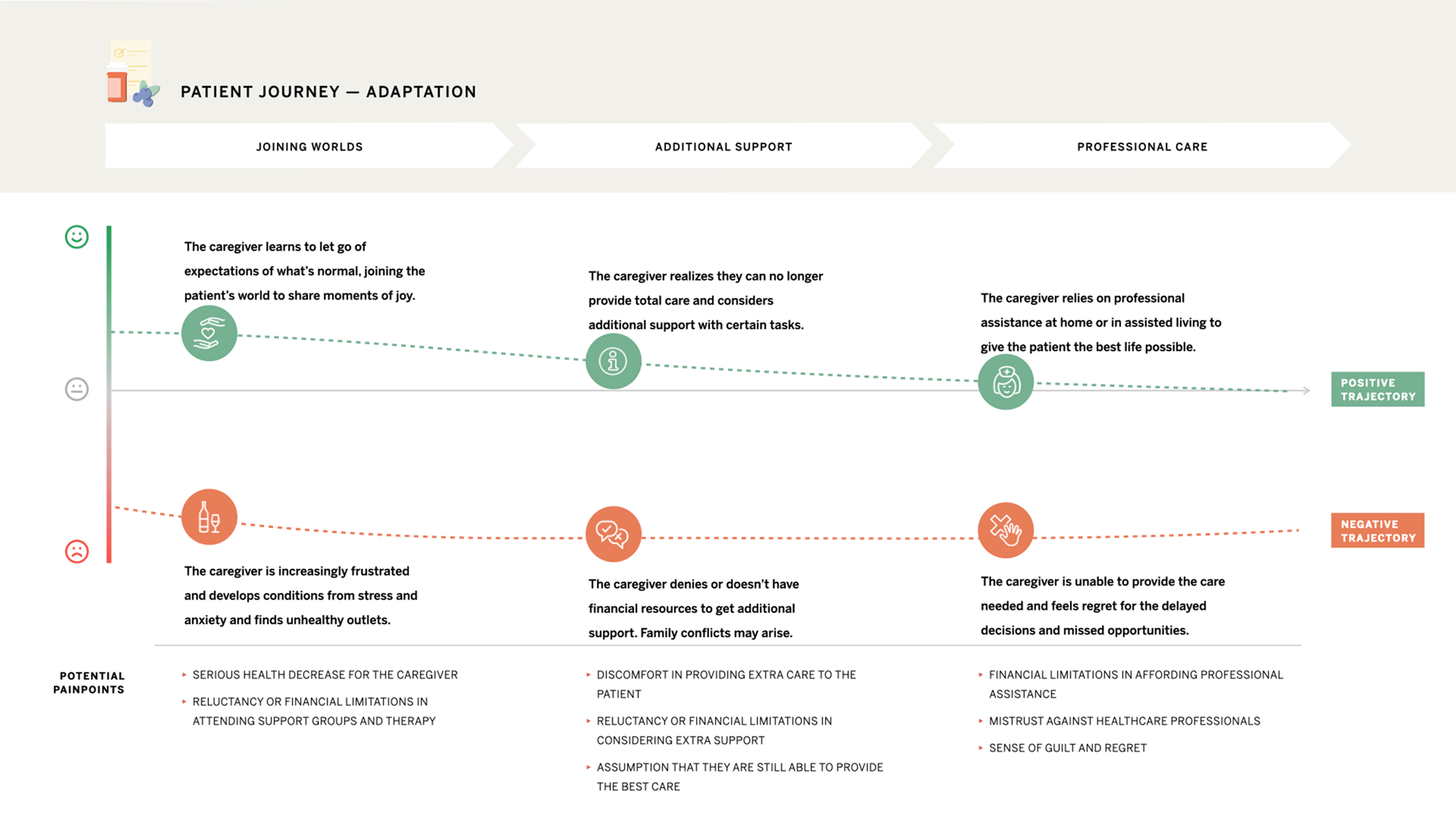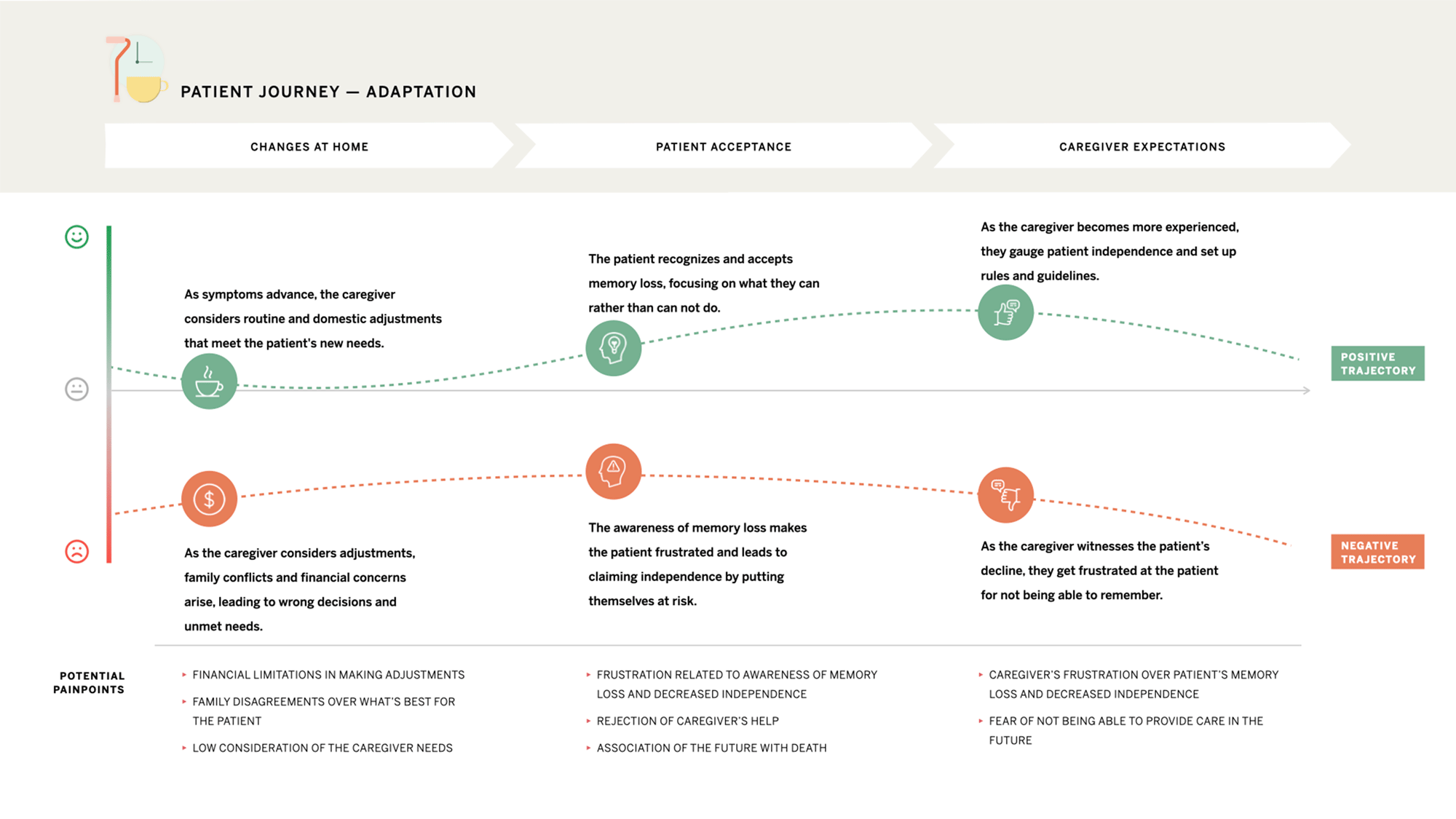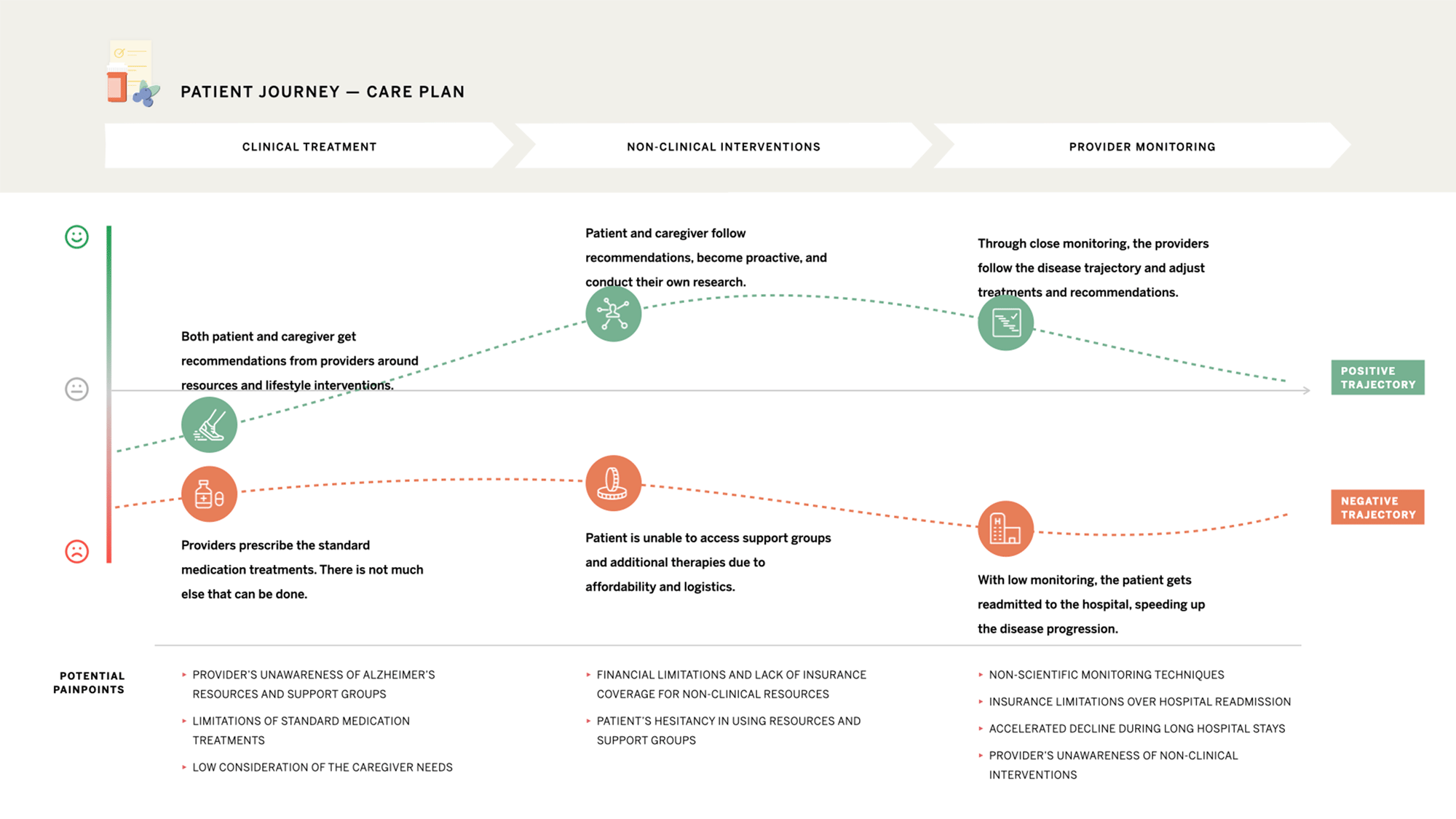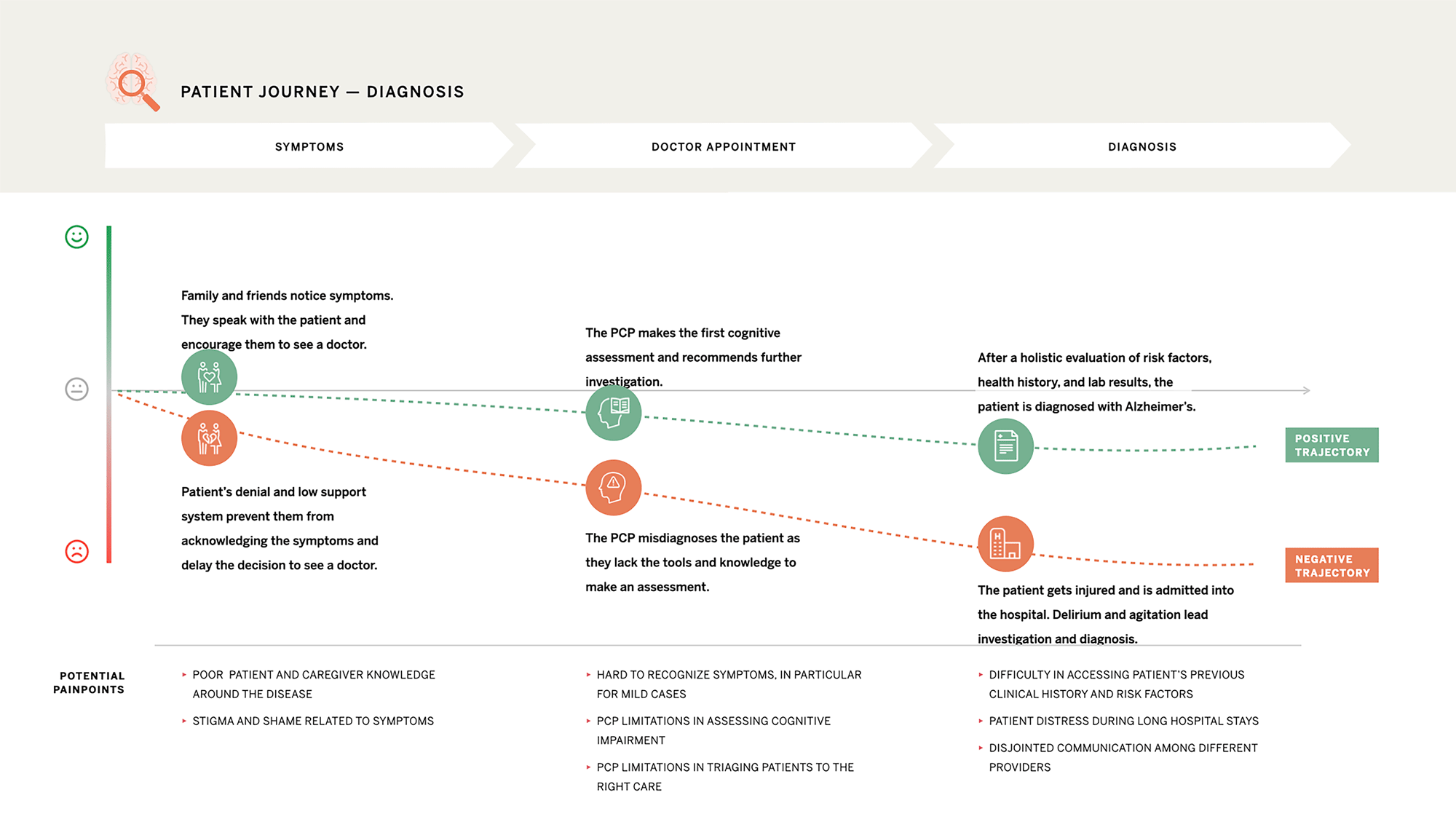
Adaptation
Defining and updating rules creates the conditions for independence and safety.
Adaptation
Routines are a double-edged sword, helpful when used selectively.
New Reality
Acceptance allows adaptation instead of a constant fight against memory change.
New Reality
Memory loss brings a special kind of grief - grieving ahead of time.
New Reality
Joining the patient’s world sparks connection and joy.
The Explorer
Identity in Doing
Priority in Independence
The Explorer is accustomed to their independence, which is their most valuable possession. They participate in activities for personal fulfillment and manage relationships on their terms - using support as needed, but hiding struggles from others. After the diagnosis, the Explorer actively tries to find solutions that empower them over their condition. They are not afraid to embrace a new normal to find purpose.
The Maximizer
Identity in Doing
Priority in Relationships
The Maximizer leverages social activities to reaffirm their identity and find purpose. They focus on what they’re still capable of and even try new things, such as traveling to new places or visiting friends and family that live far away. They don't feel shame about their struggle, and educate people in being more acceptant and understanding. Their focus is on the present; they live their best life possible and find excitement in breaking routines.

The Preserver
Identity in Memories
Priority in Independence
For the Preserver memories represent their biggest source of joy. They celebrate their stories with others and cherish what keeps them connected to their identity. Their memory loss makes them less positive about the future: not being able to remember a conversation or details from their past are reminders of the disease progression and their mortality. Their desire for independence can create conflicts with caregivers.

The Depender
Identity in Memories
Priority in Relationships
The Depender relies on close relationships and familiar environments to stay connected to their identity and feel protected. They find joy in revisiting memories and hearing from their loved ones. Their strength is knowing they are not alone. However, they may try to minimize symptoms, so to not raise concerns or feel like a burden to their caregiver. They accepted their new relationship with the family members and find comfort in their support.

Opportunity Areas
These insights revealed four strategic opportunity areas designed to support families as they navigate the transition into long-term care. The focus was to help patients accept the condition and plan for the future, bridging the gap between clinical treatments and essential community resources. By emphasizing safety and autonomy, we sought to reduce the heavy logistical burden of daily care management while simultaneously uncovering new ways for families to experience joy and connection that do not rely on cognitive recall.
Assist Adaptation
The emotional journey that comes with Alzheimer’s limits patients and caregivers from living their best life going forward.
Advocate Aurora has an opportunity to guide patients and their loved ones through the grief of an Alzheimer’s diagnosis, so they can accept the condition, prepare for change, and plan for the future to live the best life they can.
Integrate Resources
The role of healthcare in the Alzheimer’s journey is reactive and disjointed. Patients and caregivers seek out resources on their own to supplement their care.
Advocate Aurora has an opportunity to go beyond clinical treatments, connect patients to the right resources, and coordinate among them, so providers have a fuller picture of their patients’ situation and trajectory.
Ease Day-to-Day Routine
Patients and caregivers can struggle with managing everyday tasks and lifestyle interventions at home. The unpredictable nature of Alzheimer’s makes it even harder to plan for the day.
Advocate Aurora has an opportunity to reduce the burden of household and care management tasks with an emphasis on both safety and independence, so patients feel they’ve had a good day and caregivers can focus on emergent needs.
Facilitate Joy
Many people express a resigned attitude toward Alzheimer’s. Focusing on what’s been lost or the expectation of memory can prevent joyful experiences in the present.
Advocate Aurora has an opportunity to inspire patients and caregivers to break norms and find new sources of joy, as well as new ways to experience joy in their favorite activities and relationships without relying on memory.
Concept Ideation
In the final phase, I facilitated a collaborative workshop to translate these opportunities into actionable concepts. Leveraging "How Might We" prompts, the team generated a range of solutions that were prioritized through a framework balancing user desirability with core business objectives. These concepts allowed to reframe the entire care journey around "moments that matter," successfully shifting the user trajectory from a state of overwhelmed decline to a proactive and positive future experience.
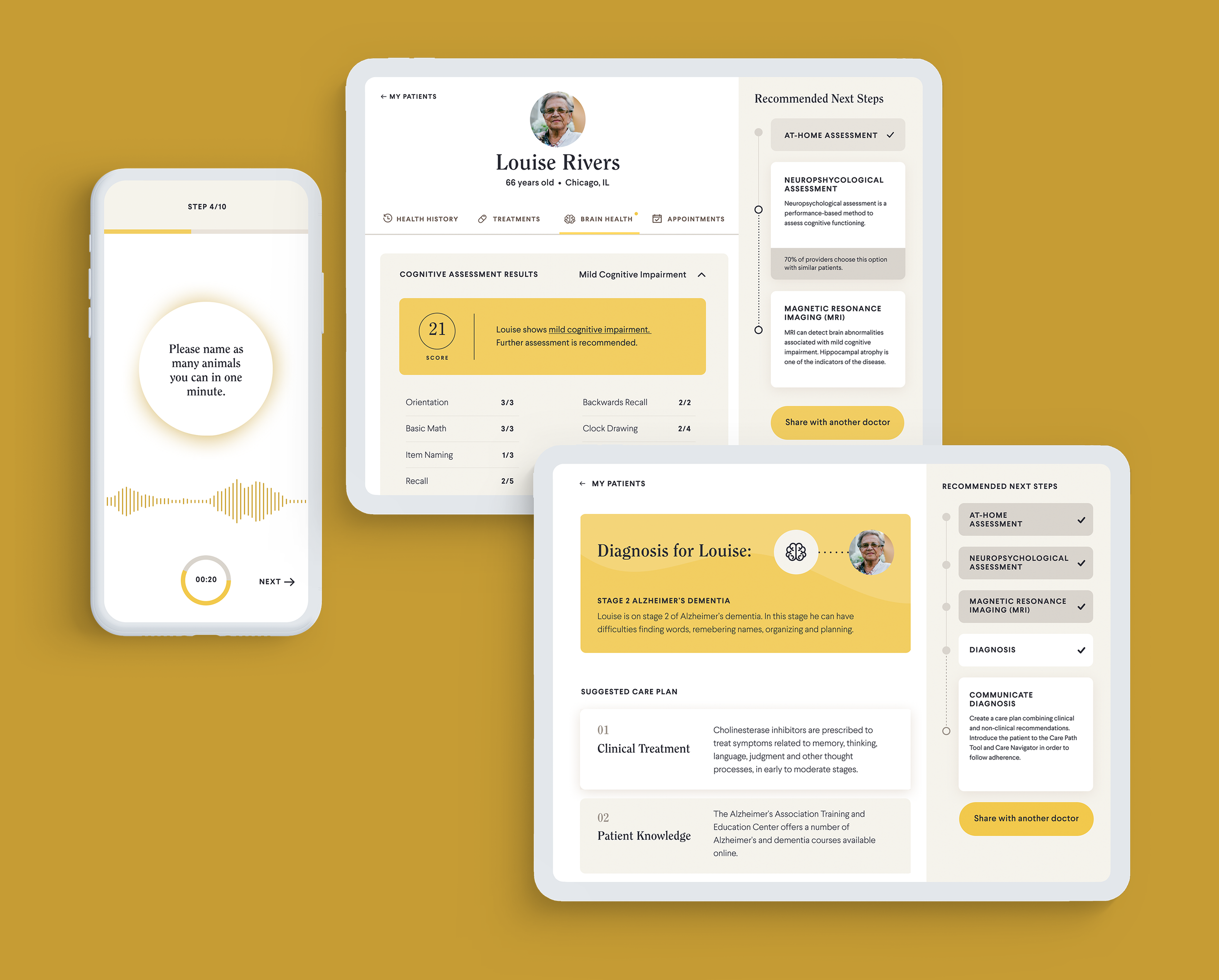
Cognitive Testing Tool
A series of touch points that leads patients to a definitive diagnosis sooner. The patient can leverage a digital at-home assessment with biometric data monitoring; collected data can be shared with the primary care doctor and visualized into a dashboard along with suggestions for next steps and support with diagnosis.
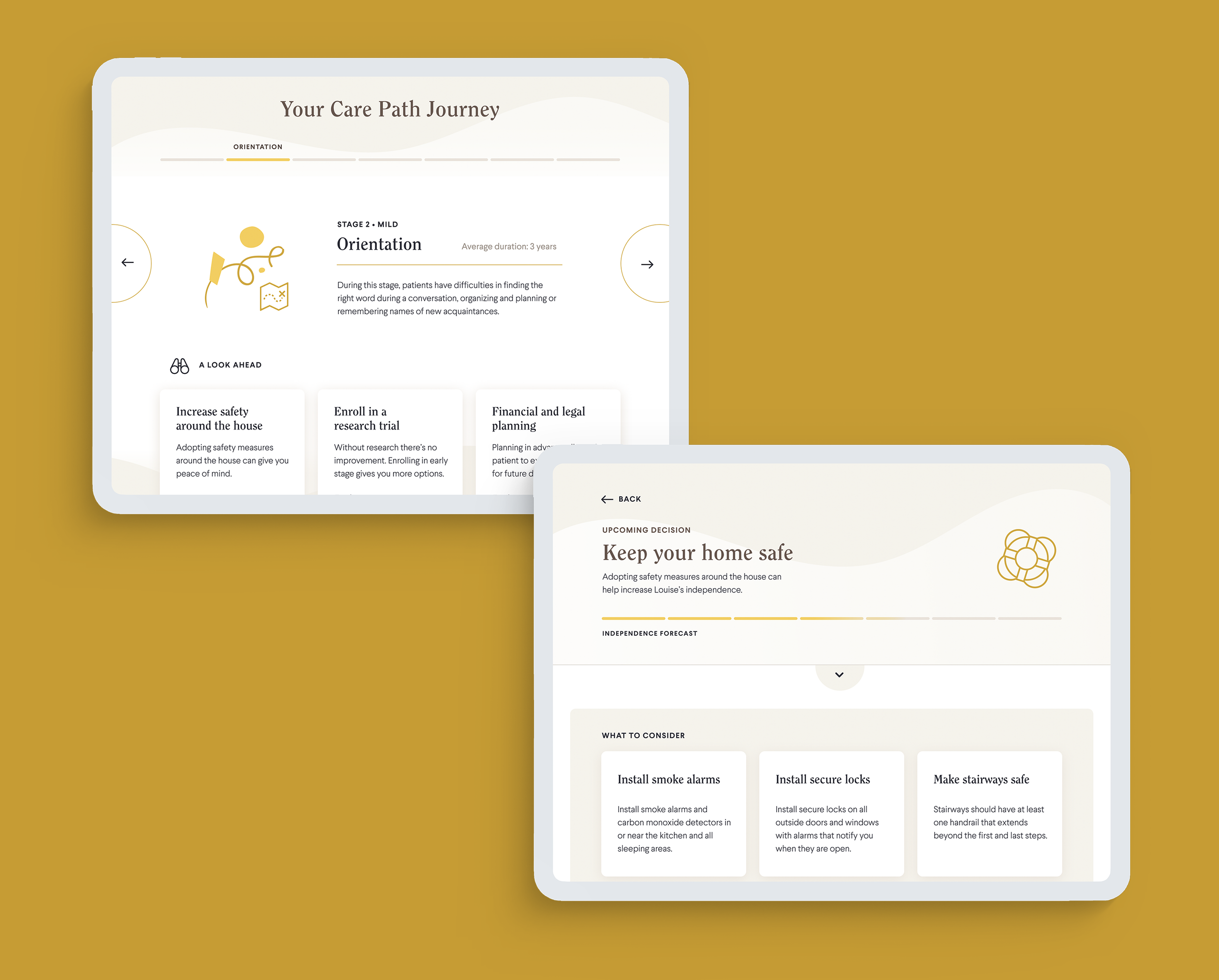
Care Path Planning Guide
An interactive digital decision tool that helps patients and their loved ones plan out future care to meet their goals. After the diagnosis, the Care Path Journey shows patients and caregivers characteristics of the disease stage, including symptoms and suggested activities. Each stage also includes decisions to consider, supported by practical considerations and implications on budget.
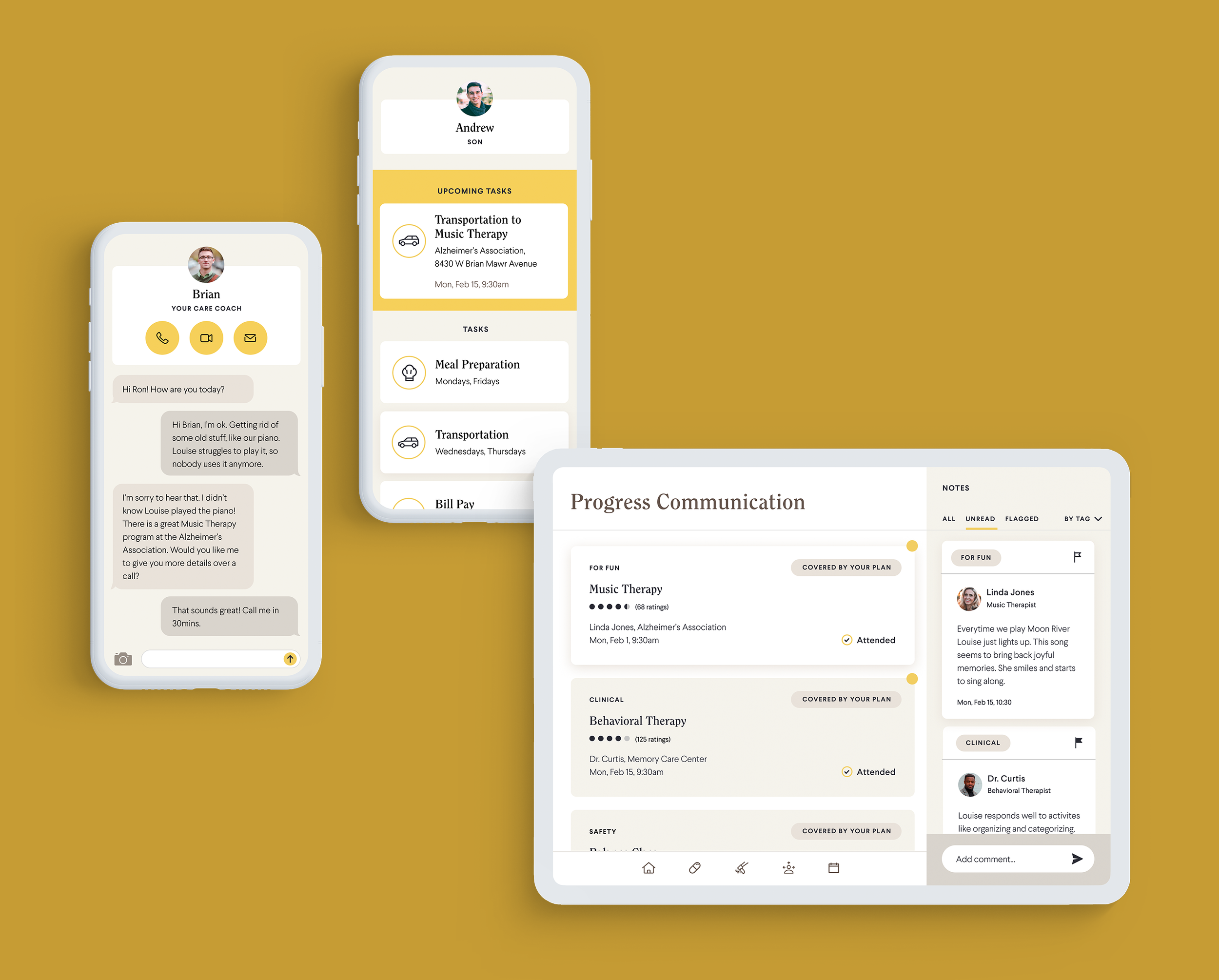
Memory Care Resource Hub
A place for families and providers to coordinate and communicate. Each family is assigned to a Care Coach for quick virtual appointments and troubleshooting to uncover new needs. The Hub captures attendance at resource appointments and notes from family members or health care providers to fill gaps among the care team.